Over 22% of Americans Likely to Experience Panic Attacks in Lifetime: A Comprehensive Look at Prevalence, Impact, and Regional Trends
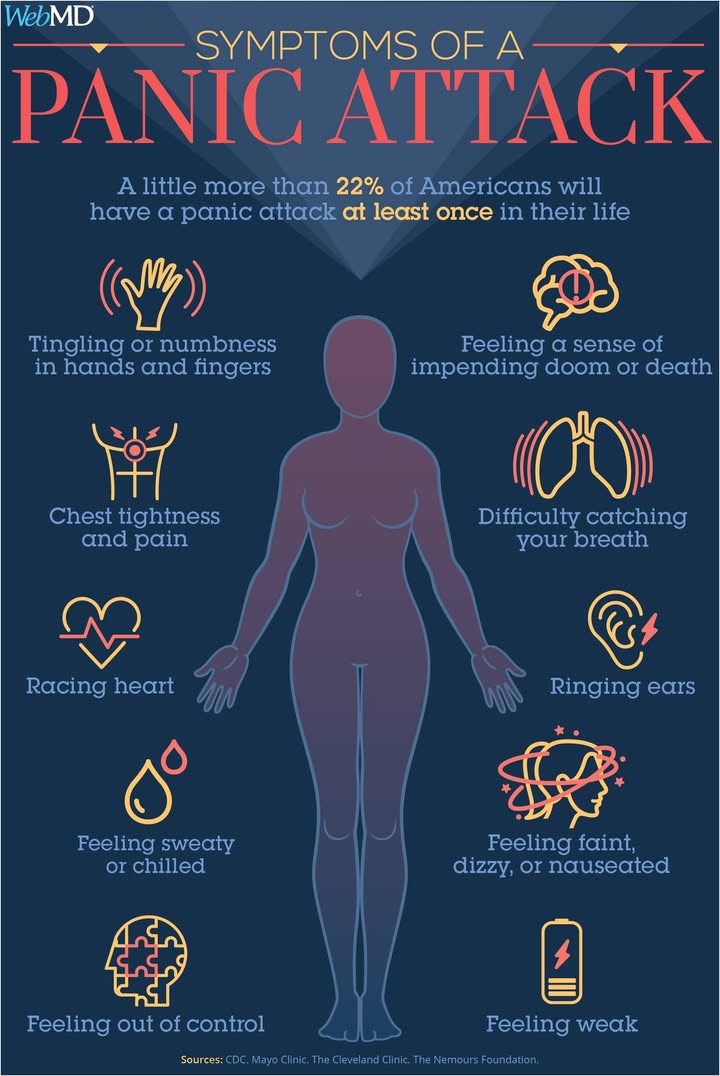
Panic attacks, sudden surges of intense fear accompanied by physical and cognitive symptoms, affect a substantial portion of the population. Recent estimates indicate that slightly more than 22% of Americans are expected to encounter at least one panic attack during their lifetime. While the experience is not uncommon, it remains a topic that blends medical insight, public health considerations, and personal narratives. This article examines the prevalence, signs, potential triggers, treatment pathways, economic implications, and regional comparisons that help contextualize panic attacks within the broader healthcare landscape.
Historical context: how perceptions of panic and anxiety evolved
Panic disorder and related episodes have long occupied a nuanced space in mental health discourse. Early twentieth-century medical writings framed intense fear responses as primarily physiological or moral concerns, often prompting stigmatization rather than understanding. The past few decades, however, have seen a shift toward recognizing panic episodes as part of a spectrum of anxiety disorders with identifiable physiological underpinnings. Advancements in neurobiology, cognitive-behavioral therapy, and pharmacology have contributed to more precise diagnosis and effective treatment pathways. This evolution reflects a broader transformation in public health: moving from silence and stigma to evidence-based care and resilience-building strategies.
Clinical signs and diagnostic considerations
A panic attack is typically defined by a sudden onset of intense fear or discomfort that peaks within minutes and is accompanied by at least four physical or cognitive symptoms. Common indicators include chest tightness or pain, rapid heartbeat, shortness of breath, dizziness or lightheadedness, sweating, trembling or shaking, tingling or numbness, a sense of unreality or detachment, fear of losing control, fear of dying, nausea, and warmth or chills. It is important to note that panic attacks can occur in individuals with or without a diagnosed panic disorder. In some cases, episodes mimic serious medical conditions, such as cardiac events, which is why differential diagnosis is essential.
Understanding triggers and risk factors
Risk factors for panic attacks are multifaceted and can involve a combination of genetics, brain chemistry, life stressors, and coping strategies. A family history of anxiety disorders increases susceptibility, as do high levels of chronic stress, traumatic experiences, or certain medical conditions. Substance use, including caffeine, alcohol withdrawal, or stimulant medications, can also contribute to attack susceptibility. Importantly, panic attacks are not a sign of personal weakness but rather a complex interplay of biological and environmental factors that may require professional support.
Regional and demographic perspectives
Prevalence estimates for panic attacks vary across regions and demographics, influenced by access to mental health care, cultural norms surrounding help-seeking, and socio-economic conditions. Urban areas with robust healthcare infrastructure may report higher reporting rates due to increased awareness and access to screening. Conversely, rural communities might exhibit underreporting due to stigma or limited resources, even as the underlying incidence remains substantial. Studies comparing regions within the United States reveal notable variations in diagnosis rates, treatment uptake, and the availability of crisis intervention services. These patterns underscore the necessity of improving access to mental health resources across the country while tailoring public health messaging to local contexts.
Economic impact and policy implications
Panic attacks and related anxiety disorders impose tangible economic costs. Direct medical expenses include primary care visits, emergency department consultations, psychiatric care, and psychotropic medications. Indirect costs encompass lost productivity, absenteeism, and disability-related supports. Employers increasingly recognize mental health as a critical component of workforce well-being, leading to broader adoption of employee assistance programs, mental health days, and on-site counseling services. Public health agencies also emphasize early intervention and prevention, recognizing that timely treatment can reduce acute care utilization and improve long-term outcomes.
Services, treatments, and best practices
Effective management of panic attacks typically involves a combination of acute coping strategies and longer-term therapeutic approaches. During an episode, grounding techniques—such as focusing on the physical environment, feeling the floor beneath the feet, or controlled breathing—can help reduce distress. Cognitive-behavioral therapy (CBT) remains a first-line treatment for many individuals, offering structured strategies to identify and reframe catastrophic thoughts, gradually expose oneself to feared situations, and develop healthier fear responses. Medications, when appropriate, may include selective serotonin reuptake inhibitors (SSRIs), serotonin-norepinephrine reuptake inhibitors (SNRIs), or, in some cases, benzodiazepines for short-term relief under professional supervision. Complementary approaches, including mindfulness-based stress reduction, regular physical activity, sleep optimization, and balanced nutrition, contribute to a holistic care plan.
Public health messaging and education
Public awareness campaigns play a critical role in reducing stigma and encouraging timely treatment. Clear communication about the signs of panic attacks, typical duration, and when to seek urgent care helps demystify the experience and empowers individuals to seek support without shame. For responders and caregivers, training in de-escalation techniques and recognizing when professionals are needed can improve outcomes for those experiencing an episode. Schools, workplaces, and community centers can implement accessible mental health resources, including crisis hotlines, on-demand counseling, and peer-support networks, to foster a supportive environment for individuals navigating anxiety-related challenges.
Regional comparisons and infrastructure considerations
When comparing regional mental health infrastructures, states with integrated care models report more seamless access to behavioral health services, early intervention programs, and coordinated care for co-occurring medical conditions. Regions investing in telemedicine and mobile crisis teams often show improved reach into underserved communities, mitigating barriers such as transportation, cost, and stigma. The economic rationale for expanding such services is strong: early and proactive management of panic symptoms can reduce emergency room visits and long-term disability, while supporting productivity and quality of life for residents.
Public health data and measurement challenges
Estimating lifetime risk for panic attacks requires careful methodological consideration. Self-report surveys may overestimate or underestimate lifetime prevalence due to recall bias, social desirability, or differences in diagnostic criteria over time. Longitudinal cohort studies help illuminate patterns of onset, progression, and remission, but they require substantial resources and consistent measurement tools. Despite these challenges, the consensus remains that panic attacks are relatively common, and their impact warrants attention within broader mental health strategies.
Historical context in today’s policies
In recent years, there has been a push to normalize conversations around mental health and to integrate mental health services within primary care settings. This integration aims to identify anxiety-related symptoms early, reduce fragmentation of care, and ensure that individuals receive comprehensive support that addresses both physical and mental health needs. Policy discussions often center on expanding access to insurance coverage for psychotherapy, reducing wait times for psychiatric assessments, and investing in community-based resources that offer culturally competent care.
Societal and cultural implications
Beyond clinical and economic factors, panic attacks influence daily life, relationships, and personal identity. Individuals may modify routines to avoid triggering environments, while families and colleagues work to provide nonjudgmental support. Understanding and empathy from communities—alongside evidence-based treatment options—play a pivotal role in helping people rebuild confidence and maintain productive lives. Public reactions to mental health discussions have evolved, reflecting broader shifts toward inclusivity and resilience in the face of mental health challenges.
Looking ahead: trends and opportunities
As awareness grows and access to care improves, the trajectory of panic attack prevalence is likely to be shaped by several forces. Advances in digital therapeutics, telepsychiatry, and data-driven personalization hold promise for more precise interventions and timely support. Environmental stressors, including economic volatility and climate-related events, may influence the frequency and intensity of panic-related symptoms, highlighting the need for adaptable mental health infrastructure. In parallel, continued investment in prevention, early intervention, and destigmatization will be essential to reduce the personal and societal burden of panic attacks.
Key takeaways
- Panic attacks affect a sizable portion of the population, with lifetime prevalence estimated just above 22%.
- Early recognition of signs and appropriate responses can mitigate distress and improve outcomes during an episode.
- A combination of evidence-based therapies, supportive care, and lifestyle practices supports long-term management.
- Regional disparities in access to care underscore the importance of expanding mental health infrastructure and leveraging local resources.
- Ongoing public education and policy initiatives aim to reduce stigma, improve access, and promote proactive mental health care.
In conclusion, the prevalence of panic attacks among Americans underscores a broader imperative: to integrate mental health care into everyday health strategies, expand access to evidence-based treatments, and foster communities that respond to anxiety with understanding and practical support. As researchers continue to deepen our understanding of the mechanisms behind panic episodes, the focus remains on empowering individuals with tools, resources, and hope to navigate these experiences with confidence and resilience.