Five Genetic Clusters Tie Mental Health Disorders to Shared Variants, Study Finds
In a sweeping genetic analysis drawing on more than a million individuals with psychiatric conditions and millions of healthy controls, researchers have identified five distinct clusters that group 14 major mental health disorders by shared genetic variants. The work, which maps thousands of genomic regions to broad categories rather than discrete diagnoses, could reshape how clinicians think about risk, diagnosis, and treatment as the field moves toward biology-guided care.
A landmark approach to psychiatric genetics The study, conducted by a coalition of researchers spanning multiple institutions, leverages large-scale genome-wide association data to search for common variants that contribute to risk across conditions. Instead of viewing disorders in isolation, the team sought patterns of genetic overlap—an approach that reflects emerging consensus in the field: many psychiatric conditions share underlying biology rather than existing as strictly separate diseases.
From the outset, investigators put the data to work in a way that mirrors how many clinicians think about patients: people often present with a constellation of symptoms that span traditional diagnostic borders. The researchers identified 238 genomic regions with associations to at least one of the five clusters, underscoring how shared biology can transcend conventional labels.
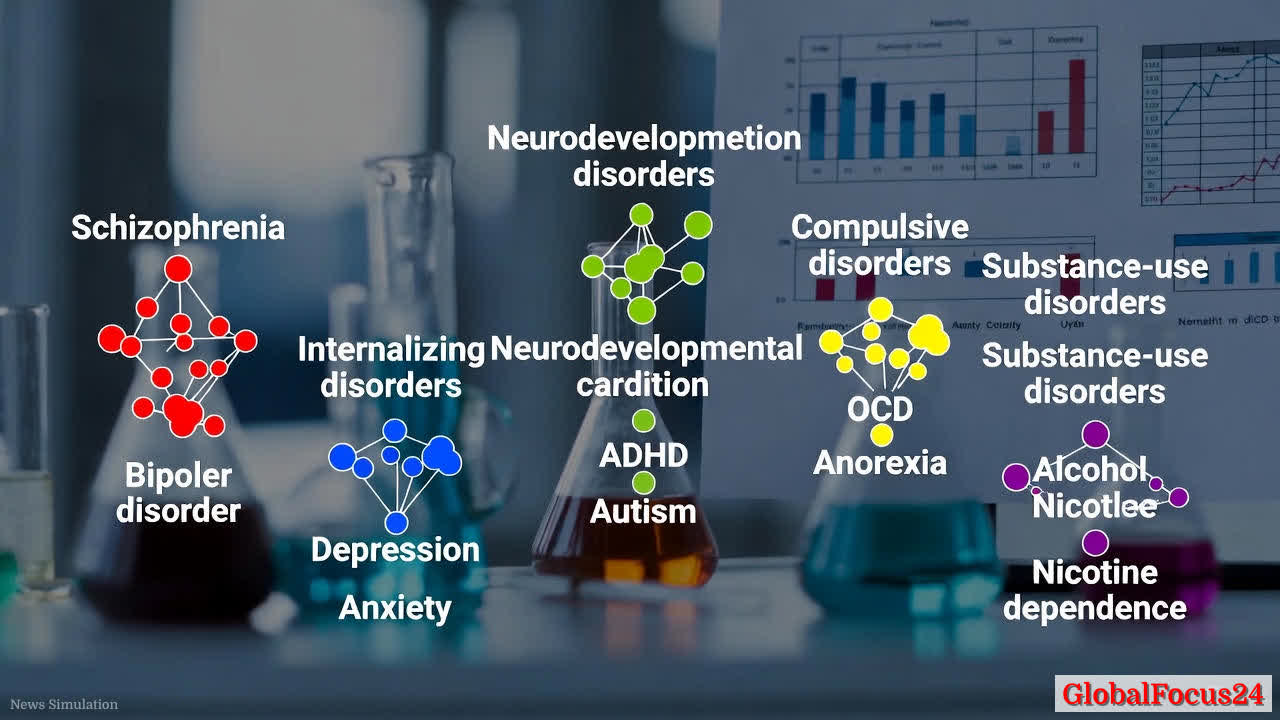
Five clusters, five biological themes
- Schizophrenia and bipolar disorder
- Internalizing disorders, including depression, anxiety, and post-traumatic stress disorder
- Neurodevelopmental conditions, such as attention deficit hyperactivity disorder and autism
- Compulsive disorders, including obsessive-compulsive disorder and anorexia
- Substance-use disorders, such as alcohol-use disorder and nicotine dependence
Within this framework, certain regions rise to prominence. For example, a region on chromosome 11 that encompasses genes involved in dopamine signaling appears to influence risk across eight different disorders. This finding highlights a core pathway that may contribute to a spectrum of psychiatric outcomes, rather than a single condition, reinforcing the idea that biology can cut across diagnostic lines.
Historical context: from categories to continua The clustering effort fits into a trajectory in psychiatric research that has challenged rigid diagnostic silos. Decades of twin and family studies have repeatedly demonstrated shared heritability among conditions once considered distinct. More recently, large consortia have shown genetic correlations between disorders such as schizophrenia and bipolar disorder, as well as between anxiety and depression. The new study extends this logic to a broader set of conditions, providing a structured map of how genetic risk concentrates within five overarching biological themes.
Experts say the work helps address a long-standing puzzle: why patients frequently exhibit comorbidity or switch between diagnoses over time. By recognizing overlapping genetic architectures, clinicians may better understand why a patient’s symptoms evolve and why a single treatment might help across multiple manifestations rather than targeting a single label.
Economic implications and potential clinical pathways The economic stakes in psychiatric care are substantial. Mental health disorders contribute to billions in both direct healthcare costs and indirect costs such as lost productivity. A framework that clarifies genetic risk and shared pathways could streamline screening and intervention, potentially reducing long-term expenses through earlier, more effective treatment strategies.
If these clusters prove robust across diverse populations, they could inform the development of precision therapies aimed at core biological processes rather than symptom-specific targets. Such a shift could accelerate the pipeline for new pharmacological agents, neuromodulation approaches, or personalized behavioral interventions that align with a patient’s underlying biology. In turn, this may influence reimbursement policies and guidelines as the healthcare system pivots toward biology-informed care.
Cross-regional comparisons and global relevance While the study aggregates data from a broad international cohort, researchers emphasize the need to validate findings across diverse populations. Genetic architectures can differ by ancestry, and environmental factors—ranging from early life stress to access to care—shape how genetic risk translates into disease. Regions with high environmental risk or limited healthcare infrastructure may experience different patterns of expression, even within the same genetic clusters.
Interpreting risk: what the clusters mean for individuals For patients and families, the five-cluster model offers a more nuanced lens through which to view mental health risk. A person with genetic variants aligning with a particular cluster may face elevated risk for any disorder contained within that group. However, environmental exposures, life experiences, and social determinants of health continue to play critical roles in actual outcomes. The study’s authors stress that genetics is a piece of a larger puzzle, not a deterministic forecast.
Public health messaging surrounding these findings is careful to balance clarity with caution. While the clustering approach can streamline conversations about risk, it does not imply inevitability. The same genetic region might contribute to multiple conditions depending on context, and protective factors can attenuate risk. Communicators emphasize that the clusters are about probabilities, not certainties.
Clinical implications: diagnostic reform and treatment targets One of the most provocative aspects of this research is the potential to simplify and refine diagnoses. By prioritizing shared genetic pathways, clinicians could move away from a proliferation of labels toward broader, pathway-based categorizations. This shift could facilitate earlier identification of individuals at risk for a cluster of disorders and enable proactive, personalized interventions tailored to underlying biology.
Moreover, treatments that target specific neural circuits or molecular pathways implicated within a cluster could offer broader applicability. If a dopamine-related region influences multiple disorders within the same cluster, therapies designed to modulate that pathway might help a range of conditions, improving efficiency in drug development and patient care.
However, experts caution that translating cluster-level insights into routine practice will take time. Rigorous replication, diverse population validation, and careful consideration of how to integrate genetic information with clinical assessment are all essential steps before changes to diagnostic manuals or treatment guidelines might be contemplated.
Regional health systems and patient communities: responses and concerns Public reaction to genetic research in psychiatry is complex and multifaceted. Some communities express hopeful anticipation that a better understanding of shared biology could reduce stigma by reframing mental illness as neurobiological in origin. Others worry about potential misuse of genetic information or discrimination in employment and insurance. Healthcare providers, policymakers, and patient advocates are engaging in ongoing conversations about informed consent, data privacy, and equitable access to any future diagnostic or therapeutic advances.
The study’s emphasis on environmental interplay serves as a reminder that genetics operates within a social world. Access to preventive resources, mental health services, and supportive community environments can modulate genetic risk. This convergence of biology and social factors underscores the importance of comprehensive public health strategies that address both biology and context.
Methodological notes and future directions The researchers employed state-of-the-art statistical genetics techniques to parse correlations across thousands of genetic variants and dozens of disorders. By identifying five principal clusters, they distilled a vast, complex landscape into a manageable framework that still captures nuanced variation. The next steps involve validating these clusters in independent cohorts, exploring gene-by-environment interactions, and examining how cluster membership relates to trajectories of illness over time.
Beyond replication, scientists aim to translate cluster insights into practical tools. This could include risk calculators that integrate genetic information with clinical and environmental data, decision-support systems for clinicians, and trials designed to stratify participants by cluster rather than by single-disease diagnosis. If successful, such tools could accelerate the discovery of effective interventions and help patients receive targeted care sooner.
Background on genetic pathways and key regions A notable highlight of the study is the identification of regions that recur across disorders within a cluster. The chromosome 11 region linked to dopamine signaling, for example, points to a central mechanism—dopaminergic pathways—known to influence reward processing, motivation, and executive function. Dysregulation in these circuits has long been implicated in multiple psychiatric conditions, lending credence to the clustering approach.
Other regions likely involve genes tied to synaptic development, neurotransmitter regulation, and neural connectivity. While individual variants often exert modest effects, their collective action across networks shapes vulnerability to psychiatric illness. The integration of these signals into coherent clusters represents a significant step in translating polygenic risk into actionable biology.
Public-health implications: monitoring, screening, and prevention From a population health perspective, the clusters offer a framework for contemplating screening priorities and preventive interventions. For instance, communities disproportionately affected by certain environmental stressors might benefit from targeted programs that address modifiable risk factors while leveraging genetic insights for early detection. Public health agencies could use cluster-informed strategies to design evidence-based, culturally appropriate mental health campaigns and services.
Ethical considerations and responsible communication As with any genetic research touching on mental health, ethical considerations are paramount. Researchers and clinicians must navigate issues around consent, the potential for stigmatization, and the responsible communication of probabilistic information. Efforts to educate the public about what cluster membership implies—and does not imply—are essential to prevent misinterpretation and misuse.
A future of integrated care The five-cluster model represents a promising step toward integrating genetic insights with clinical practice. By revealing shared biology across disorders, the research lays groundwork for a more unified understanding of mental health. As science advances, clinicians may be better equipped to tailor interventions to an individual’s biological profile, bridging the gap between psychiatric genetics and everyday patient care.
In the broader arc of psychiatric research, this work aligns with a growing trend: moving from a legacy of siloed diagnoses toward a holistic appreciation of brain function and its disruption. The ultimate goal remains clear: reduce suffering, improve outcomes, and provide care that reflects the complexity of human mental health in real-world settings.
Background on the study’s collaboration and data scope The study leveraged multiple large-scale datasets, combining clinical information with genetic data from a diverse, global population. By integrating data across cohorts, researchers increased statistical power to detect cross-disorder signals and ensure robustness of the five-cluster framework. The emphasis on replication and cross-population validation remains a cornerstone of advancing these findings toward clinical utility.
Public reaction and immediate takeaways Early responses from patient groups and healthcare professionals highlight a mix of cautious optimism and measured skepticism. Many express relief that research is moving toward a comprehensive view of mental health that recognizes interconnected biology. Others reiterate that the translation to clinical practice will require careful validation, equitable access to testing and care, and ongoing dialogue about how best to support people through risk, diagnosis, and treatment.
Future outlook: what comes next Looking ahead, researchers aim to validate the five-cluster model in independent datasets, refine the mapping of specific genetic variants to each cluster, and investigate how cluster membership interacts with life experiences, socioeconomic factors, and treatment responses. If subsequent work confirms and extends these findings, the clustering framework could become a standard lens through which clinicians assess risk and design personalized care plans for mental health conditions.
Key takeaways for readers
- A vast genetic study identifies five clusters that group 14 major mental health disorders by shared genetic variants.
- The chromosome 11 region involving dopamine signaling exemplifies cross-disorder influence within a cluster.
- The clustering approach holds promise for simplifying diagnosis and guiding treatments that target underlying biological pathways.
- Environmental factors and social determinants of health remain critical in shaping actual outcomes.
- Ongoing validation, ethical considerations, and careful communication are essential as science progresses toward clinical application.
In summary, the five-cluster architecture marks a meaningful advancement in psychiatric genetics. By reframing how disorders relate to each other at the genetic level, researchers are laying groundwork for a future in which mental health care is more integrated, biology-informed, and potentially more effective for patients across a spectrum of conditions. As the field advances, clinicians, researchers, and communities will watch closely how these insights translate from genomic maps into real-world care, with the shared aim of alleviating suffering and improving lives.