Pneumonia: Symptoms, Causes, Treatment, and Prevention of a Serious Lung Infection
What Is Pneumonia and Why It Matters
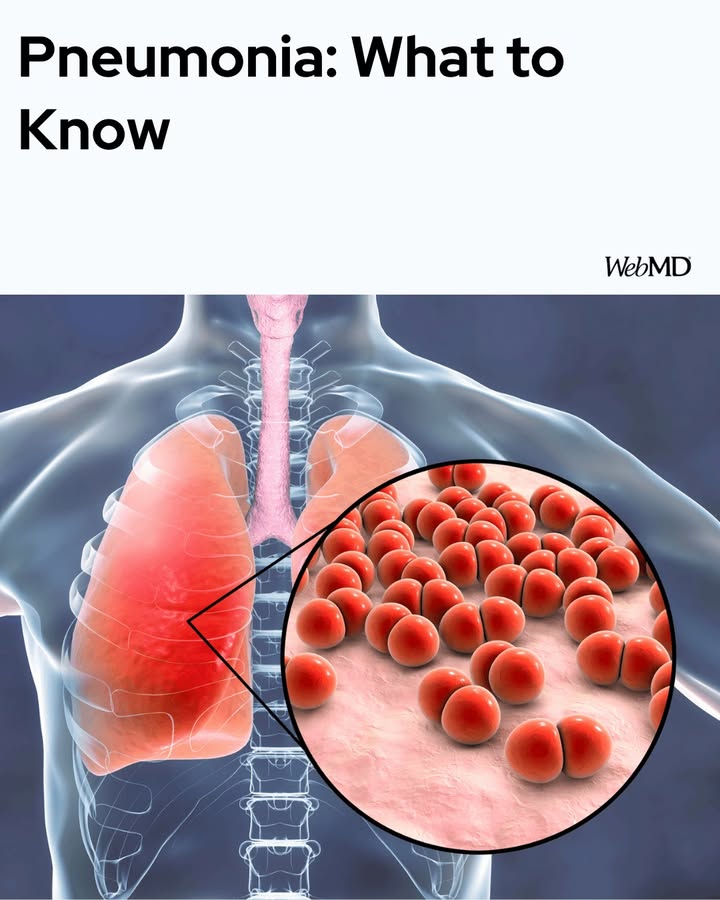
Pneumonia remains one of the most widespread and potentially serious respiratory infections globally, affecting millions of people each year across all age groups. The condition develops when infections inflame the air sacs in the lungs, causing them to fill with fluid or pus. This disrupts the body’s ability to absorb oxygen efficiently, leading to breathing difficulties that can range from mild discomfort to life-threatening complications.
Although pneumonia can affect anyone, certain populations—including infants, older adults, and individuals with weakened immune systems—face a significantly higher risk of severe illness. The disease continues to place a considerable burden on healthcare systems worldwide, especially during peak respiratory virus seasons.
Historical Context and Global Burden
Pneumonia has long been a leading cause of death, particularly before the widespread use of antibiotics in the 20th century. In the early 1900s, it was often referred to as “the old man’s friend” because it frequently claimed the lives of elderly individuals. The introduction of antibiotics and vaccines dramatically reduced mortality rates, yet pneumonia remains a major global health challenge.
According to global health estimates, pneumonia is still one of the top infectious killers, especially among children under five in developing regions and adults over 65 in industrialized nations. Seasonal surges, often linked to influenza outbreaks or emerging respiratory viruses, continue to strain hospitals and healthcare resources.
Causes and Types of Pneumonia
Pneumonia can arise from several types of infectious agents, each with distinct characteristics and treatment approaches.
- Bacterial pneumonia is the most common form, often caused by Streptococcus pneumoniae. It may develop suddenly and is sometimes preceded by a cold or flu.
- Viral pneumonia accounts for a substantial portion of cases, particularly in children. Common viruses include influenza, respiratory syncytial virus (RSV), and SARS-CoV-2.
- Fungal pneumonia is less common but can occur in individuals exposed to environmental fungi, especially those with weakened immune systems.
- Aspiration pneumonia results from inhaling food, liquid, or vomit into the lungs, often affecting people with swallowing difficulties.
- Hospital-acquired pneumonia develops during hospital stays and can involve antibiotic-resistant bacteria, making it more difficult to treat.
- Ventilator-associated pneumonia occurs in patients using mechanical breathing support.
- Walking pneumonia is a milder form, typically caused by atypical bacteria, and often allows individuals to continue daily activities despite infection.
Each type varies in severity, contagiousness, and treatment requirements, making accurate diagnosis critical.
Symptoms and Warning Signs
Pneumonia symptoms can vary widely depending on the cause, age, and overall health of the individual. In some cases, symptoms may be subtle or mistaken for a common cold.
Common signs include:
- Persistent cough, often producing mucus or phlegm
- Shortness of breath or difficulty breathing
- Chest pain that worsens with coughing or deep breathing
- Fever, chills, and sweating
- Fatigue and weakness
- Loss of appetite
- Rapid breathing or heartbeat
- Nausea, vomiting, or diarrhea
In more severe cases, symptoms may include confusion, bluish lips or fingernails (indicating low oxygen levels), or significant respiratory distress.
Children and infants may show different signs, such as difficulty feeding, restlessness, or unusual sleepiness. Older adults may experience confusion or a drop in body temperature rather than a fever, making diagnosis more challenging.
How Pneumonia Spreads
Many forms of pneumonia spread through respiratory droplets when an infected person coughs, sneezes, or talks. These droplets can be inhaled directly or transferred via contaminated surfaces.
However, not all types are contagious. Fungal pneumonia and aspiration pneumonia typically arise from environmental exposure or internal factors rather than person-to-person transmission.
The ease of transmission, especially in crowded environments such as schools, workplaces, and healthcare facilities, contributes to periodic outbreaks.
Diagnosis and Medical Evaluation
Diagnosing pneumonia involves a combination of clinical assessment and diagnostic testing. Healthcare providers typically begin with a physical examination, listening for abnormal lung sounds such as crackling or wheezing.
Additional diagnostic tools may include:
- Chest X-rays to identify lung inflammation or fluid buildup
- Blood tests to detect infection and assess severity
- Pulse oximetry to measure oxygen levels in the blood
- Sputum tests to identify the causative organism
- CT scans or bronchoscopy in complex or severe cases
Early and accurate diagnosis is essential to guide appropriate treatment and prevent complications.
Treatment Options and Recovery
Treatment for pneumonia depends on its underlying cause and severity. While mild cases may resolve with home care, more serious infections require medical intervention.
- Bacterial pneumonia is treated with antibiotics, which must be taken for the full prescribed duration.
- Viral pneumonia typically involves supportive care such as rest, hydration, and fever management, though antiviral medications may be used in certain cases.
- Fungal pneumonia requires antifungal medications, often administered over an extended period.
Severe cases may require hospitalization, where treatment can include:
- Intravenous antibiotics or fluids
- Oxygen therapy to support breathing
- Respiratory treatments to open airways
- Drainage procedures if fluid accumulates around the lungs
Recovery time varies, ranging from one week for mild cases to several weeks or longer for more severe infections. Fatigue can persist even after other symptoms improve.
Economic and Healthcare Impact
Pneumonia imposes a substantial economic burden, both directly through medical costs and indirectly through lost productivity. Hospitalizations, particularly among older adults, are a major driver of healthcare expenses.
In the United States alone, pneumonia leads to hundreds of thousands of hospital admissions annually. The costs associated with inpatient care, medications, and follow-up treatment contribute to billions of dollars in healthcare spending each year.
Globally, the impact is even more pronounced in low- and middle-income countries, where limited access to vaccines, antibiotics, and healthcare infrastructure leads to higher mortality rates.
Regional Comparisons and Risk Patterns
The prevalence and severity of pneumonia vary by region due to differences in healthcare access, vaccination rates, environmental conditions, and population demographics.
- In high-income regions such as North America and Europe, pneumonia is more common among older adults and individuals with chronic conditions. Advanced healthcare systems help reduce mortality rates.
- In low-income regions, particularly parts of Sub-Saharan Africa and South Asia, children under five face the highest risk due to limited access to vaccines and medical care.
- Urban areas with high pollution levels may experience increased respiratory vulnerability, contributing to higher incidence rates.
- Seasonal variations also play a role, with cases typically rising during colder months when respiratory viruses spread more easily.
Understanding these patterns helps guide public health strategies and resource allocation.
Prevention Strategies and Vaccination
Preventing pneumonia involves a combination of lifestyle practices, public health measures, and vaccination.
Key prevention steps include:
- Frequent handwashing to reduce exposure to infectious agents
- Avoiding close contact with individuals who are sick
- Covering coughs and sneezes properly
- Cleaning frequently touched surfaces
- Quitting smoking and avoiding secondhand smoke
- Managing chronic health conditions effectively
Vaccination plays a central role in prevention, particularly for high-risk populations. Vaccines are available to protect against several pneumonia-related pathogens, including:
- Pneumococcal bacteria
- Influenza viruses
- COVID-19
- Haemophilus influenzae type b (Hib)
- Respiratory syncytial virus (RSV)
- Measles and whooping cough
Widespread immunization has significantly reduced the incidence of severe pneumonia in many parts of the world.
Complications and When to Seek Care
If left untreated or if severe, pneumonia can lead to serious complications, including:
- Bacteria entering the bloodstream (sepsis)
- Respiratory failure requiring mechanical ventilation
- Fluid accumulation around the lungs
- Lung abscess formation
- Acute respiratory distress syndrome (ARDS)
- Kidney failure or worsening heart conditions
Prompt medical attention is essential if symptoms worsen or do not improve within a few days. Warning signs such as difficulty breathing, persistent high fever, or confusion require immediate evaluation.
Early treatment significantly improves outcomes and reduces the risk of long-term complications.
A Continuing Public Health Concern
Despite advances in medicine, pneumonia remains a major cause of illness and death worldwide. Its ability to affect vulnerable populations, strain healthcare systems, and cause severe complications underscores the importance of awareness, prevention, and timely treatment.
Ongoing efforts in vaccination, early diagnosis, and improved access to care continue to play a critical role in reducing the global burden of this common but potentially life-threatening lung infection.