Vitamin B12 Deficiency Signals Surge in Health Screenings as Demand for Testing Rises
Subhead: A wake-up call for millions, with symptoms spanning fatigue, neurological changes, and digestive discomfort prompting more people to seek evaluation and treatment
Health officials are reporting a noticeable uptick in inquiries about vitamin B12 deficiency in recent months, as more individuals seek medical advice after experiencing a cluster of symptoms that can be subtle, gradual, and easy to overlook. Medical professionals say the condition, which affects red blood cell formation, nerve function, and DNA synthesis, presents across a spectrum—from mild fatigue to more pronounced neurological and cognitive changes—creating a growing need for awareness, timely testing, and accessible treatment options. The pattern aligns with broader public health trends, including aging populations, changing dietary patterns, and rising attention to nutrient health as part of routine wellness checks.
Historical context: how B12 became central to modern nutrition Vitamin B12, or cobalamin, has long been recognized as a crucial micronutrient for human physiology. Discovered in the mid-20th century, B12’s essential role in red blood cell production and neurological maintenance has driven decades of research and clinical practice. In the late 20th century, as vegetarian and vegan diets gained popularity for ethical, environmental, and health reasons, clinicians began detailing the risk of deficiency in individuals who avoid animal products. The current wave of testing and supplementation reflects a convergence of two enduring threads: well-documented clinical pathways for diagnosing and treating deficiency, and an increasingly empowered consumer base seeking proactive, preventive care.
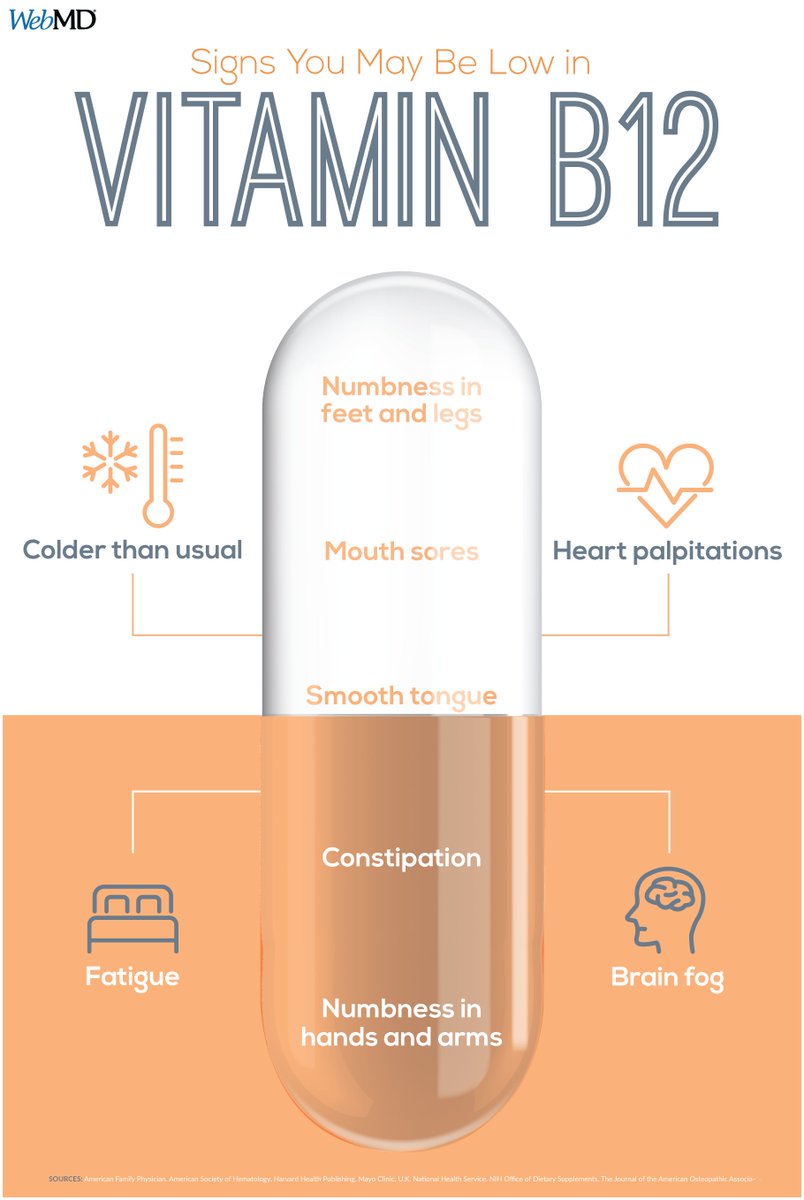
What symptoms are most concerning, and why they matter Health professionals emphasize that vitamin B12 deficiency can present with a wide range of signs, which may appear gradually and be mistaken for other conditions. Persistent fatigue remains one of the most commonly reported symptoms, stemming from the body's diminished capacity to generate energy from glucose efficiently. For some patients, the fatigue is severe enough to disrupt daily activities, work performance, and sleep patterns.
Neurological symptoms often appear as numbness or tingling in the hands, arms, feet, and legs. This “pins and needles” sensation can progress if not addressed, potentially affecting balance, coordination, and fine motor skills. In some cases, patients describe a sensation of electric-like shocks or a burning feeling in extremities, particularly after exposure to heat or cold.
Digestive issues also feature prominently. People may experience constipation or diarrhea, and mucosal changes in the mouth can produce mouth sores or a smooth, glossy tongue that may be sore or sensitive to acidic foods. In severe cases, digestion-related symptoms accompany other signs, signaling the importance of a comprehensive clinical evaluation rather than isolated self-diagnosis.
Cognitive and mental health concerns are increasingly documented in relation to B12 deficiency. Patients may report brain fog, difficulty focusing, short-term memory lapses, or a sense of mental cloudiness. While such symptoms can overlap with other conditions, clinicians now view B12 status as a potential contributing factor in holistic cognitive health, particularly in older adults.
Cardiovascular and circulatory impacts, though less common in everyday reports, can include heart palpitations or an unusual sensitivity to temperature. These indicators reflect the nutrient’s role in energy metabolism and nerve function, which indirectly influence cardiovascular efficiency and thermal regulation.
Regional and demographic patterns: who is most at risk Specific populations face higher risks of deficiency, prompting targeted screening strategies. Older adults are commonly advised to monitor B12 levels, given age-related changes in stomach acid production that can hinder absorption. Vegans and vegetarians, who exclude most or all animal products, are another high-risk group due to dietary sources being primarily animal-based. People with certain gastrointestinal disorders, such as pernicious anemia, Crohn’s disease, celiac disease, or those who have undergone intestinal surgery, may also experience malabsorption, increasing the likelihood of deficiency. Additionally, individuals on long-term proton pump inhibitors or metformin therapy may face absorption challenges, underscoring the need for periodic assessment in patients using these medications.
Economic impact: testing, treatment, and broader costs The surge in awareness translates into economic implications across healthcare systems. Routine screening for vitamin B12 levels—often part of a broader metabolic or wellness panel—can lead to earlier detection, which in turn reduces the risk of complications that require more intensive care. The cost of testing is typically borne by patients or insurers, with laboratory analyses commonly measuring serum B12 concentration, methylmalonic acid (MMA), and homocysteine as complementary markers when results are ambiguous.
Treatment options, including dietary adjustments and supplementation, have measurable effects on healthcare spending. For many patients, oral B12 supplements or fortified foods restore function with relatively low annual costs, particularly when compared to the long-term expenses associated with unmanaged deficiency. In some instances, clinicians prescribe high-dose injections to bypass absorption issues, a practice that carries its own logistical and staffing considerations but can dramatically improve outcomes for individuals with significant malabsorption.
Public health initiatives and regional comparisons Public health campaigns in several regions have prioritized nutrient status as a component of general wellness, recognizing that B12 deficiency, if left unchecked, can lead to anemia, neuropathy, and cognitive decline. Some countries with robust food fortification programs—designed to add B12 to common staples—report lower prevalence of overt deficiency, though gaps remain among subpopulations with limited access to fortified products or specific dietary patterns. In areas with higher rates of vegetarian or vegan populations, healthcare providers emphasize education about fortified foods and reliable supplementation to prevent deficiency.
Comparative patterns across regions reveal that urban centers often have greater access to testing and specialty care, while rural communities may face barriers related to distance, provider shortages, and insurance coverage. These disparities influence both the timeliness of diagnosis and the initiation of treatment, underscoring the need for scalable, equitable screening programs and telemedicine options where appropriate.
What diagnostics reveal: interpreting blood tests and when to seek care A definitive diagnosis typically begins with a blood test to measure serum vitamin B12 levels. However, because B12 status can be influenced by factors such as binding proteins and recent dietary intake, doctors may also evaluate metabolites like methylmalonic acid (MMA) and homocysteine. Elevated MMA or homocysteine in the context of borderline B12 levels can support a diagnosis of deficiency, guiding clinicians toward supplementation or further investigation.
Clinicians commonly differentiate between true deficiency and functional deficiency, where B12 is present but not effectively utilized due to issues at the cellular level. In such cases, treatment decisions may rely on a combination of laboratory markers, clinical presentation, and patient history rather than a single test result.
Public health messaging emphasizes that symptoms alone should not be the sole basis for diagnosis; rather, they should prompt a clinical evaluation that includes history-taking, dietary assessment, and appropriate laboratory testing. Early detection is important because timely intervention can reverse or mitigate many symptoms, particularly fatigue, cognitive concerns, and some neuropathic signs.
Diet, lifestyle, and practical steps for prevention Dietary sources rich in B12 include animal products such as meat, fish, dairy, and eggs, with fortified cereals and plant-based milks serving as important alternatives for those following vegetarian or vegan diets. For adults not at risk of malabsorption, a balanced diet that includes fortified foods or an appropriate supplement can help maintain adequate levels. Nutrition experts often recommend a daily intake that aligns with established dietary guidelines, tailored to age, health status, and lifestyle.
Lifestyle considerations also play a role. Alcohol use, certain medications, and gastrointestinal health influence B12 absorption and reserves in the body. Individuals at higher risk may benefit from periodic screening, especially if they notice symptoms like fatigue, numbness, or cognitive changes. Healthcare providers commonly advise maintaining a nutrient-rich diet and discussing supplementation with a clinician to determine the correct dosage and form, such as cyanocobalamin or methylcobalamin, based on individual needs and absorption considerations.
Public reaction and future directions Public awareness campaigns have highlighted the importance of recognizing early, sometimes subtle, symptoms of B12 deficiency. Patients reporting persistent fatigue, neuropathic sensations, and cognitive concerns are increasingly encouraged to consult healthcare professionals for a comprehensive evaluation. The narrative around B12 health also intersects with broader conversations about nutrition, aging, and preventive care, reinforcing the idea that nutrient status is a foundational element of overall well-being.
Researchers continue to explore the nuanced relationship between B12 status and brain health, noting that cognitive function in older adults may be affected by long-standing deficiencies and that timely treatment can result in meaningful improvements. Public health advocates emphasize the importance of accessible testing, affordable supplementation, and education for at-risk groups to minimize long-term health impacts and enhance quality of life.
Conclusion: a practical path forward for individuals and systems The rising attention to vitamin B12 deficiency signals a broader shift toward proactive nutrient management as part of routine health care. For individuals, recognizing the signs—especially fatigue, numbness or tingling, digestive changes, and cognitive shifts—can prompt earlier testing and intervention. For health systems, expanding access to affordable testing, fortification programs, and consumer education can reduce the burden of deficiency-related complications and support healthier aging.
As the conversation around nutrition evolves, vitamin B12 remains a cornerstone nutrient whose proper management offers a clear, tangible path to improved energy, nerve health, and cognitive function for millions of people worldwide. Public health data, clinical guidelines, and patient experiences collectively underscore the practical imperative: ensure reliable access to testing, understand dietary sources and supplementation options, and normalize nutrient-status checks as a standard component of preventive care.