Understanding Bipolar Depression: Causes, Symptoms, and Paths to Treatment
Recognizing the Dual Nature of Bipolar Disorder
Bipolar disorder, historically referred to as manic-depressive illness, is a complex mental health condition that affects mood, energy levels, and the ability to function in daily life. It is characterized by alternating periods of mania or hypomania—episodes of elevated mood and increased activity—and depression, marked by persistent sadness and fatigue. Among the two poles of this condition, bipolar depression often proves most debilitating.
Unlike ordinary mood swings, bipolar depression can last for weeks or months and may significantly impair professional performance, relationships, and quality of life. For many, the depressive phase becomes the dominant expression of the disorder, often leading to misdiagnosis as major depressive disorder. Understanding its specific symptoms and patterns is essential for accurate diagnosis and effective treatment.
The Core Symptoms of Bipolar Depression
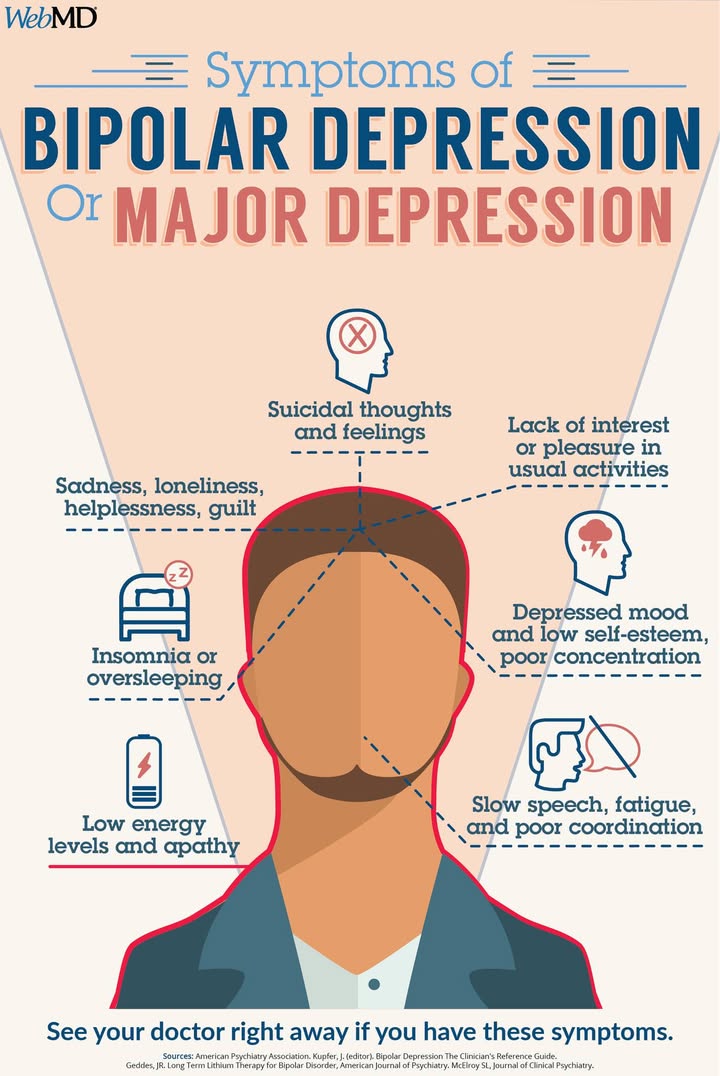
The primary symptoms of bipolar depression extend beyond sadness or low energy. Individuals often experience prolonged feelings of hopelessness or emptiness, loss of interest in once-enjoyable activities, and difficulty focusing on daily tasks. Common features include:
- Persistent low mood or feelings of sadness and apathy
- Loss of self-esteem or feelings of excessive guilt
- Fatigue, lethargy, or physical slowing
- Cognitive impairment such as poor concentration and indecision
- Changes in sleep patterns—either insomnia or excessive sleeping
- Disrupted appetite, leading to noticeable weight changes
- Suicidal thoughts or preoccupation with death
These symptoms may fluctuate in severity but often leave the individual feeling immobilized, drained, or emotionally numb. Unlike unipolar depression, periods of recovery may be followed by manic or hypomanic episodes—periods of excessive energy, impulsivity, and sometimes decreased need for sleep. This alternating pattern defines the cyclical nature of the disorder.
Historical Perspectives on Bipolar Depression
References to conditions resembling bipolar disorder date back to ancient Greek medicine, when physicians such as Aretaeus of Cappadocia described mood states of “melancholia” and “mania” within the same individual. In the 19th century, French psychiatrists Jules Falret and Jean-Pierre Baillarger formally distinguished “circular insanity,” recognizing the alternating cycles of mania and depression.
The modern term bipolar disorder entered psychiatric vocabulary in the late 20th century as understanding of brain chemistry advanced. Researchers began identifying potential links between neurotransmitter imbalances, genetics, and environmental stressors. This historical evolution reflects a shift from moral or character-based interpretations of mood disturbances to a biological and psychological understanding of mental illness.
In recent decades, the growing visibility of mental health advocacy has helped demystify bipolar depression. Well-known public figures sharing their personal experiences have encouraged greater acceptance and earlier treatment. Yet, despite progress, many people still face stigma or delay seeking help due to misconceptions about the disorder’s seriousness or treatability.
Global Prevalence and Regional Comparisons
Bipolar disorder affects an estimated 1 to 3 percent of the global population, with varying rates across regions due to cultural, diagnostic, and systemic differences. In North America, improved awareness and access to psychiatric care have led to higher detection rates compared to developing regions. The United States, for instance, reports lifetime prevalence close to 2.8 percent among adults, according to major mental health surveys.
In Europe, national healthcare systems have adopted standardized screening programs, resulting in earlier diagnosis and greater access to mood-stabilizing medications. However, in parts of Asia, Africa, and Latin America, underreporting remains a challenge. Limited mental health infrastructure, cultural stigma, and lack of psychiatric training can prevent individuals from receiving a clear diagnosis or continuous care.
Despite these disparities, clinicians worldwide note similar symptom patterns and life-long cycles. Studies suggest that genetics account for up to 80 percent of an individual’s risk, indicating that bipolar depression crosses borders, languages, and cultures.
Economic and Societal Impact
The economic burden of bipolar depression extends far beyond healthcare costs. Individuals may experience job loss, reduced productivity, or disability due to unpredictable mood shifts and prolonged depressive episodes. A 2025 global mental health report estimated that mood disorders, including bipolar depression, contribute to substantial losses in workforce participation, with ripple effects on families and communities.
In the United States, the annual economic cost of bipolar disorder exceeds tens of billions of dollars, encompassing medical expenses, lost wages, and social service dependency. Employers increasingly invest in workplace mental health programs to reduce absenteeism and support affected employees through flexible work arrangements and counseling benefits.
The societal toll also includes strain on relationships and increased risk of substance misuse, often used by individuals to self-medicate against emotional extremes. These coping mechanisms, while temporarily numbing distress, can worsen symptoms over time and increase the complexity of treatment.
Understanding the Biological and Psychological Roots
Advancements in neurobiology have deepened our understanding of bipolar depression. The condition appears linked to irregularities in neurotransmitters such as serotonin, dopamine, and norepinephrine—chemical messengers that regulate mood and energy. Structural brain imaging has identified subtle differences in the prefrontal cortex and amygdala, regions involved in emotional regulation.
Genetic research reveals that first-degree relatives of bipolar individuals carry a markedly higher risk, though no single “bipolar gene” has been identified. Instead, a combination of genetic variations, early life experiences, and chronic stress appear to converge in altering brain function.
Psychological factors such as trauma, loss, or prolonged stress can trigger or exacerbate episodes. Lifestyle patterns—irregular sleep, substance use, or disrupted daily routines—often play a role in maintaining instability. Because of its multifactorial nature, bipolar depression requires integrated care addressing both biological and psychosocial dimensions.
Diagnosis and Challenges in Treatment
Diagnosing bipolar depression is often complex because its depressive episodes resemble those of unipolar depression. Clinicians rely on detailed patient histories to identify subtle indicators of past hypomanic episodes—periods of elevated mood, decreased need for sleep, or impulsive behavior. Without these details, the condition may be mislabeled, leading to treatment plans that fail to stabilize mood.
Treatment typically involves a combination of medication and psychotherapy. Mood stabilizers such as lithium, anticonvulsants, and certain antipsychotic drugs remain the cornerstone of pharmacological management. These medications help prevent mood swings and reduce the risk of relapse. Antidepressants may be used cautiously and usually in combination with stabilizers, as they can sometimes trigger mania if used alone.
Psychotherapeutic approaches, including cognitive-behavioral therapy (CBT), interpersonal therapy, and family-focused therapy, reinforce medication adherence and teach coping strategies. Regular routines, sleep hygiene, and stress management also play crucial roles in maintaining stability.
Public Awareness and Shifts in Perception
Public awareness of bipolar depression has grown significantly in recent years. Educational campaigns, mental health apps, and online support networks have made information more accessible than ever before. Universities and workplaces increasingly offer counseling resources, reflecting a broader societal recognition that mental wellness is integral to overall health.
However, barriers remain. Misunderstandings about the disorder’s nature can lead to stigma, isolation, or discrimination. Many individuals still hesitate to disclose their diagnosis for fear of being perceived as unstable or unreliable. Experts emphasize that destigmatizing language—focusing on “living with” rather than “suffering from” bipolar disorder—encourages recovery-oriented narratives.
Community-based programs have also proven effective. Peer-led support groups, crisis hotlines, and educational workshops provide essential spaces for individuals to share experiences, build resilience, and access early intervention.
Looking Ahead: A Future of Hope and Stability
Medical research continues to refine treatment options for bipolar depression. New-generation medications targeting specific neural pathways, combined with digital monitoring tools such as smartphone-based mood tracking, offer promise for personalized care. Advances in genomic and neuroimaging studies may eventually allow clinicians to predict vulnerability and tailor therapies more precisely.
As mental health rises on global public health agendas, early detection and long-term management will remain priorities. Despite its chronic nature, bipolar depression does not define a person’s potential or quality of life. With consistent treatment, social support, and self-awareness, many individuals live stable and fulfilling lives.
The growing recognition that mental health is as vital as physical health marks an important cultural shift. Bipolar depression, though complex and often misunderstood, represents one of modern medicine’s most navigable frontiers—one where science, compassion, and community converge to restore balance to the human mind.