Frequent Nightmares Linked to Higher Premature Mortality and Accelerated Biological Age, Study Finds
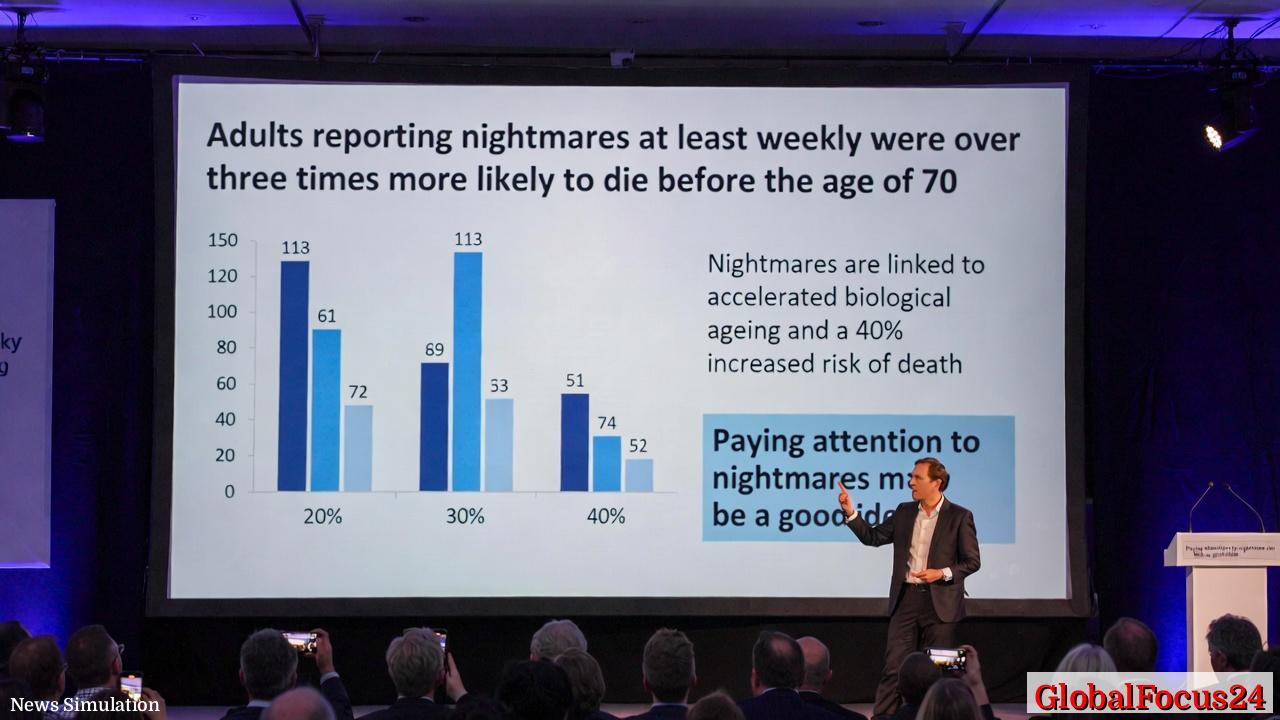
In a landmark analysis spanning more than 180,000 adults and 2,400 children across several long-term cohorts, researchers have identified frequent nightmares as a significant independent predictor of premature death. The study, presented at a European neurology congress, found that adults who reported experiencing nightmares at least once a week were more than three times as likely to die before age 70 compared with those who rarely or never sleep with such distressing dreams. The findings add a startling dimension to public health discussions, suggesting that nocturnal distress may reflect deeper physiological processes tied to ageing and overall mortality risk.
A comprehensive look at the data reveals that the relationship between nightmares and lifespan persists even after adjusting for a wide array of health conditions and lifestyle factors. This strengthens the argument that nightmare frequency operates independently of traditional risk drivers such as smoking, obesity, poor diet, and insufficient physical activity. The study also showed that even monthly nightmares correlate with faster biological ageing, measured through shorter telomeres and accelerated epigenetic aging clocks. Alarmingly, these markers of ageing explained roughly 40 percent of the observed increase in mortality risk associated with frequent nightmares.
Historical context: nightmares in medical literature have long fascinated researchers because they straddle mental health and physiological processes. For decades, clinicians have noted that chronic sleep disturbances can accompany mood disorders, stress, anxiety, and trauma. However, the new findings push the envelope by quantifying nightmares as a stand-alone prognostic indicator for longevity, independent of comorbid conditions. The shift echoes a broader trend in medicine that treats sleep health as a foundational pillar of well-being. Historically, sleep research has evolved from a focus on sleep duration to a more nuanced understanding of sleep quality, architecture, and the cascade of systemic effects triggered by disruptive sleep patterns. This study adds a new chapter to that narrative, highlighting the potential for nightmares to reflect underlying biological processes linked to cellular ageing and mortality risk.
Economic impact: the potential implications for health systems and workplace productivity are noteworthy. If nightmares serve as a proxy for accelerated ageing and higher mortality risk, early identification and intervention could hypothetically reduce healthcare utilization and associated costs over time. Employers, insurers, and public health authorities may take an interest in sleep wellness programs, stress management strategies, and sleep disorder screenings as part of comprehensive health initiatives. While the findings do not imply that nightmares cause death, they do suggest that addressing sleep disturbances could contribute to broader longevity and healthspan goals, thereby influencing long-term economic planning and resource allocation within healthcare systems.
Regional comparisons: patterns of sleep health exhibit regional variation driven by socioeconomic factors, daylight exposure, work culture, and access to mental health services. In some regions, higher reported nightmare frequency correlates with urban stressors, shift work, and crowded living conditions, while other areas with robust healthcare infrastructure report better sleep quality despite high population density. Cross-regional analyses can illuminate how environmental and policy differences shape sleep health and, by extension, mortality risk. Such comparisons may also guide tailored public health messaging that emphasizes sleep hygiene, mental health support, and early screening for sleep disorders as part of regional health strategies.
Biological ageing mechanisms: the study’s emphasis on telomere length and epigenetic clocks points to concrete biological pathways linking nightmares to ageing processes. Telomeres, protective caps at chromosome ends, shorten with cellular replication and stress, serving as a biomarker of cellular ageing. Epigenetic clocks measure DNA methylation patterns that correlate with biological age, often diverging from chronological age in response to health and lifestyle factors. The observed acceleration in these markers among those with frequent nightmares suggests that nocturnal distress may reflect chronic stress responses, sympathetic nervous system activation, or inflammatory processes that hasten cellular ageing. This biological framing helps explain why nightmare frequency could translate into higher mortality risk, even when conventional risk factors are controlled for.
Public health implications: the absence of immediate clinical guidance should not overshadow the importance of sleep health. Healthcare providers can integrate simple sleep assessments into routine care, asking patients about nightmare frequency as part of a broader sleep quality questionnaire. When frequent nightmares are reported, clinicians might consider evaluating for underlying sleep disorders, anxiety, trauma-related conditions, or depressive symptoms, as well as lifestyle factors that contribute to sleep disruption. Interventions that have demonstrated value in improving sleep quality—cognitive-behavioral therapy for insomnia (CBT-I), stress reduction techniques, and consistent sleep schedules—could conceivably mitigate some of the associated risks, though further research is needed to establish causal links and the effectiveness of specific treatments on long-term mortality outcomes.
Guidance for individuals: maintaining a regular sleep routine, creating a calming bedtime environment, and managing stress are practical steps that can contribute to better sleep quality. If nightmares are frequent and distressing, seeking evaluation from a sleep specialist or mental health professional may be appropriate. Therapeutic approaches—ranging from imagery rehearsal therapy to certain forms of psychotherapy—have shown promise in reducing nightmare frequency and improving overall sleep health. Although the study does not claim that nightmares directly cause early death, addressing sleep disturbances can be a valuable component of a proactive health strategy.
Regional health policy considerations: policymakers could consider integrating sleep health into public health priorities, especially in populations with high baseline stress or shift-work schedules. Community sleep clinics, workplace wellness programs, and educational campaigns about sleep hygiene might help raise awareness and destigmatize sleep-related concerns. Investments in mental health resources, stress management, and access to sleep medicine specialists could create a more resilient public health framework, potentially influencing long-term health outcomes and life expectancy trends.
Methodology and study scope: the research aggregated longitudinal data from diverse cohorts, allowing for robust analysis of nightmare frequency and mortality risk over extended follow-up periods. By combining adult and child data, the study offers a broader perspective on how nocturnal distress manifests across age groups. The researchers employed objective biomarkers of ageing, such as telomere length and epigenetic age estimators, to quantify biological ageing alongside traditional survival analyses. Importantly, the study’s design accounted for a range of health conditions and risk modifiers, lending credibility to the conclusion that nightmares can operate as an independent predictor.
Implications for future research: the findings open several avenues for exploration. Longitudinal studies could examine whether interventions that reduce nightmare frequency translate into measurable improvements in telomere integrity or epigenetic age trajectories. Investigations into sex-specific differences, genetic predispositions, and environmental modifiers could refine understanding of who is most at risk and why. Additionally, integrating sleep data with metabolic, cardiovascular, and inflammatory biomarkers may yield a more comprehensive model of how nocturnal distress interfaces with systemic ageing processes. If replicated and extended, these results could influence screening practices and early preventive strategies across healthcare systems.
Public reaction and media framing: the study has sparked discussion about sleep as a legitimate cardiovascular and longevity-related risk factor, paralleling established attention given to blood pressure, cholesterol, and physical activity. Public interest in sleep health is surging as more people recognize the impact of nightly rest on daily functioning and long-term wellbeing. Whiles may emphasize the magnitude of the association, health communicators stress the importance of avoiding deterministic conclusions; instead, they advocate for viewing nightmares as a possible signal of broader sleep and mental health concerns that deserve attention and treatment when needed.
Illustrative example: imagine a city where a significant portion of the population reports recurrent nightmares. Municipal health departments could collaborate with employers to implement sleep-friendly workplace policies, provide access to sleep clinics, and promote mental health resources. Over time, if such programs reduce nightmare frequency and improve sleep quality, communities might observe downstream benefits—fewer sick days, better cognitive performance, and gradual improvements in population-level indicators of ageing. This thought experiment underscores how sleep health intersects with public welfare and economic vitality.
In sum, the study elevates the conversation around sleep health by identifying frequent nightmares as an independent predictor of premature mortality and accelerated biological ageing. While causes and consequences remain complex, the implications for research, clinical practice, and public health policy are clear: prioritizing sleep quality, addressing nocturnal distress, and expanding access to sleep-related care could contribute to healthier ageing trajectories and potentially extend healthy life expectancy for diverse populations.
Would you like this article tailored for a specific publication style or audience, such as a medical journal, business readership, or general audience outreach?