Federal Elderly Programs Reach Historic Spending Peak, Facing Long-Term Sustainability Challenges
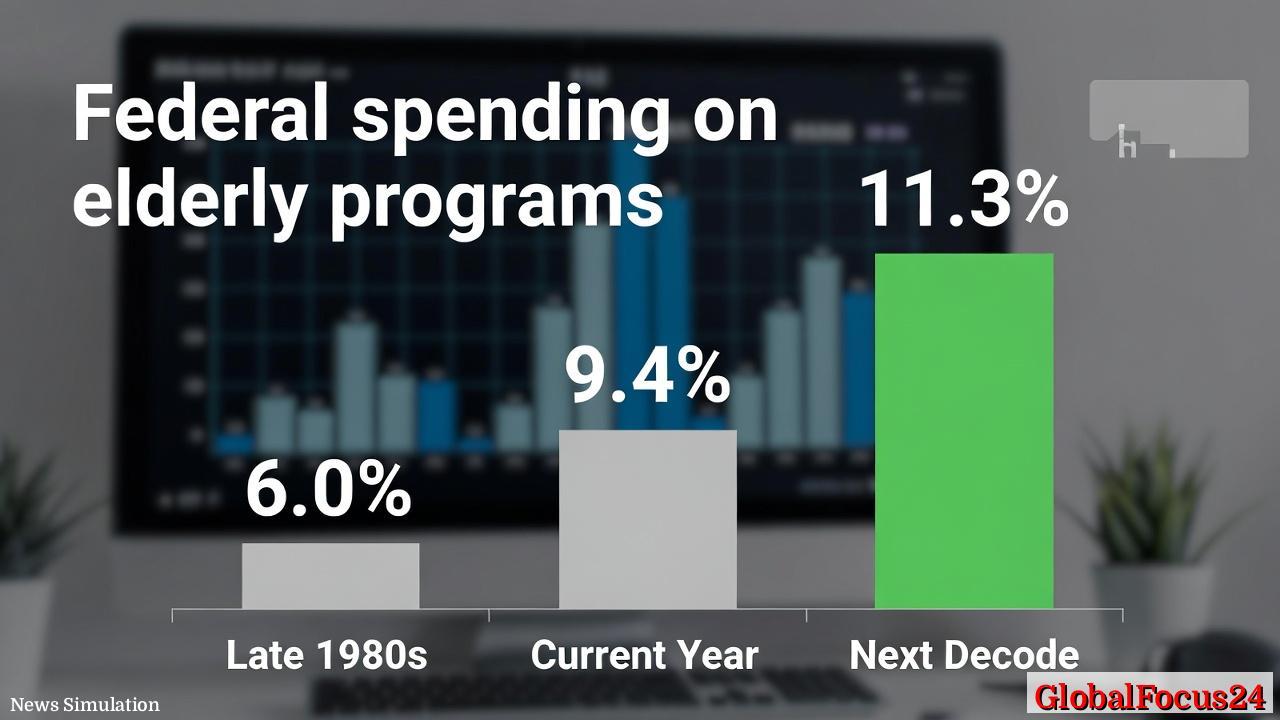
Executive summary Federal spending on elderly programs has surged to a record share of the economy, signaling a pivotal shift in the country’s fiscal landscape. At 9.4% of gross domestic product (GDP) today, up from 6.0% in the late 1980s, these programs are projected to climb to 11.3% of GDP over the next decade. Factors driving the rise include healthcare inflation, longer life expectancies, and aging demographics, which together stretch the fiscal envelope and reshape budget tradeoffs. By the early 2030s, structural pressures threaten the ability to deliver full Social Security benefits without policy reform. The broader context includes the impact on regional economies, interest payments, and the potential need to reimagine retirement security for a growing cohort of seniors.
Historical context: from postwar expansion to modern fiscal pressures The United States has a long arc of expanding social insurance programs, with elderly benefits occupying a central role for generations. In the late 20th century, reforms and relatively stable demographics kept costs manageable, even as healthcare costs began a steep ascent. New allowances, a growing workforce, and advances in medical technology contributed to longer life spans and better living standards for retirees. Yet as the baby-boom generation aged into eligibility, the aging of the population accelerated fiscal pressures. The late 1980s marked a turning point, when federal spending on elder programs as a share of GDP hovered around 6.0%—a level that reflected both program generosity and a relatively youthful population with lower dependency demands. Since then, a combination of rising healthcare costs, slower productivity growth in some healthcare sectors, and increasing life expectancy has shifted the cost curve decisively upward.
Current spending and near-term trajectory Recent fiscal data show elder programs consuming a record and rising portion of the nation’s economic output. At 9.4% of GDP today, these programs are not only a reflection of policy design but also a mirror of demographic realities: more retirees drawing benefits for longer periods, a larger elderly population relative to workers, and the ongoing inflation that bleeds into medical pricing. Healthcare inflation remains one of the most potent accelerants of this trend. Hospitals, pharmaceuticals, long-term care, and chronic disease management all contribute to sustained cost pressure, even as other parts of the economy experience mixed inflation dynamics.
Projections for the next decade point to continued growth in the elderly bill. By 2032, the projected share of GDP devoted to elderly programs climbs to about 11.3%. This increment implies hundreds of billions of dollars in additional annual spending by the federal government, depending on economic growth, policy actions, and healthcare cost trajectories. The combination of rising expenditures and existing debt service obligations means that elderly programs have become a central driver of the federal budget deficit, a shift some economists describe as structural rather than cyclical.
Life expectancy, benefits duration, and demographic realities Life expectancy for Americans aged 65 reached 19.7 years in 2024, a milestone that translates into longer periods of benefit receipt. Extended lifespans mean more years of Social Security, Medicare, Medicaid, and related programs funded by payroll taxes, general revenues, and bond markets. The longer retirees draw benefits, the more pronounced the intergenerational transfer dynamic becomes: younger workers fund a larger share of benefits via payroll taxes, while a growing segment of the population depends on those benefits for longer durations. This dynamic complicates attempts to stabilize the system through straightforward spending cuts or revenue increases alone.
Regional and economic impact The fiscal strain from elderly programs has a significant regional dimension. States with higher shares of elderly residents—often in the Sun Belt, the Pacific Northwest, and aging Northeast corridors—experience elevated demand for healthcare services, long-term care infrastructure, and pension-related spending. Conversely, regions with younger demographics may face different budget pressures, balancing the needs of schools, infrastructure, and innovation ecosystems against rising healthcare costs. Local economies in retirement hubs may see consumer demand shift toward services that cater to aging populations, while tax bases adapt to federal changes in entitlements and transfer payments.
Economic and market implications
- Interest payments: As the government borrows to finance rising deficits, interest payments on the national debt represent another mounting pressure. These costs can crowd out other priorities, potentially constraining discretionary spending and investments in infrastructure, research, and education.
- Inflation and wage dynamics: Persistent healthcare inflation feeds broader price growth and can influence wage negotiations, labor mobility, and the cost structure of the public and private sectors. Employers, insurers, and providers all adjust pricing and coverage strategies in response to policy signals and cost trajectories.
- Capital markets and fiscal credibility: Prolonged deficits tied to elder programs can affect national saving rates, bond yields, and the perceived sustainability of long-term entitlement commitments. Market discipline may influence policy choices as investors weigh the longevity of funding mechanisms and the risk of abrupt reform.
Policy options and reform considerations Policy makers face a suite of options to address the rising cost curve while preserving essential protections for seniors. These options often require careful calibration to balance fiscal sustainability with social commitments and economic growth. Some avenues under discussion include:
- Medicare structure adjustments: Modest changes to benefit design, cost-sharing, or provider payment rates can influence the trajectory of healthcare spending without necessarily reducing access to essential services.
- Social Security reform: Proposals frequently focus on a mix of gradual benefit adjustments, extended payroll tax bases, or changes to benefit formulas to ensure solvency over the medium to long term. Complementary measures, such as delayed eligibility age or targeted relief for low-income beneficiaries, are often part of reform packages.
- Tax policy and revenue enhancements: Broadening the tax base, adjusting marginal rates, or modifying payroll tax contributions can help finance rising elder costs, while preserving incentives for work and investment.
- Long-term care investment: Expanding public-private partnerships, expanding home- and community-based services, and incentivizing private long-term care coverage can reduce hospital and institutional care costs while improving quality of life for beneficiaries.
- Efficiency and innovation in care delivery: Leveraging digital health, telemedicine, care coordination, and data analytics can reduce waste and improve outcomes, potentially lowering per-capita costs over time.
Comparisons with peer economies Similar fiscal dynamics appear in many advanced economies facing aging populations. Countries with robust universal or mixed health and pension systems often grapple with rising old-age spending, balancing defense of benefits with the imperative to maintain competitiveness and fiscal credibility. In some cases, governments have pursued gradual, phased reforms designed to preserve core social protections while accelerating efficiency and cost containment in healthcare and pensions. Regional comparisons highlight the importance of early planning, transparent governance, and the role of labor markets in shaping pension solvency and healthcare access.
Public reaction and societal implications Public sentiment around elderly programs tends to be highly nuanced. For many, these programs are a lifeline—fundamental to financial security in retirement. For others, rising costs provoke concerns about intergenerational fairness, tax burdens, and the possibility of changing eligibility criteria. The sense of urgency around reform is often tempered by political realities and the desire to protect vulnerable populations. Amid this tension, policymakers emphasize transparency, stakeholder engagement, and phased reforms to maintain trust and stability in the retirement system.
National policy considerations and governance At the federal level, the sustainability of elderly programs hinges on a mix of policy levers, including entitlement design, revenue structure, and debt management. Coordination across agencies—Social Security Administration, the Centers for Medicare and Medicaid Services, and the Office of Management and Budget—becomes crucial as reforms unfold. Transparent budgeting, long-range forecasting, and independent oversight help ensure reforms are evidence-based and responsive to changing demographics and medical innovations.
Implications for future budgeting and planning As elder program costs rise, the federal budget will increasingly reflect long-term commitments rather than short-term priorities. This shift calls for robust fiscal planning, credible reform timetables, and engagement with the public about tradeoffs. The interdependence between retirement benefits, healthcare access, and general economic health means that effective policy must address not only dollars and deficits but also the lived experiences of seniors who rely on these programs.
Conclusion: a turning point in fiscal stewardship The current trajectory of federal spending on elderly programs marks a critical juncture in the nation’s fiscal story. The combination of higher life expectancy, persistent healthcare inflation, and an aging population creates a structural challenge that extends beyond annual budgets. To maintain the integrity of Social Security, Medicare, and related programs while sustaining economic growth, policymakers will need to balance reform with compassion, ensuring that retirees retain dignity and security. Regions across the country will feel the impact in distinct ways, underscoring the importance of targeted, thoughtful approaches that recognize local realities alongside national budgetary realities. The coming decade offers an opportunity for measured reform—designed to preserve essential protections, strengthen fiscal credibility, and support a dynamic economy that adapts to an aging but active population.