Overdose Deaths Are Falling in America: A Shift in the Nation’s Drug Crisis
After more than a decade of relentless escalation, the United States is witnessing a striking reversal in drug-overdose deaths. The trend, which once seemed unstoppable, is now moving downward for the first time in years. Public health officials, researchers, and communities across the country are beginning to see the results of both structural shifts in the drug market and intensified prevention efforts. The new data, reflecting 12-month moving totals through 2025, suggest that overdose deaths have plunged from over 110,000 at their peak around 2023 to roughly 70,000 by 2025—a decline of nearly 40 percent in just two years.
This unexpected turnaround marks one of the most significant public health developments of the past decade. It offers cautious optimism that the deadliest phase of the opioid epidemic may finally be easing, though other forms of substance use continue to pose serious challenges.
The Long Rise to Crisis
The roots of the current drug overdose crisis stretch back to the late 1990s, when prescription opioids began flooding American medicine cabinets. Overprescribing, coupled with aggressive pharmaceutical marketing, propelled widespread dependency. By the early 2010s, crackdowns on prescription opioids inadvertently drove many dependent users toward heroin, which was cheaper and increasingly available. Around 2015, a new, more lethal wave emerged—synthetic opioids, principally fentanyl, entered the market.
Deaths surged as fentanyl began contaminating not only heroin but also cocaine, counterfeit prescription pills, and methamphetamine. National overdose fatalities climbed sharply, from about 50,000 in 2015 to more than 110,000 by 2023. Fentanyl became the leading cause of death for Americans aged 18 to 45, far surpassing car crashes and gun violence.
A Sudden and Sustained Decline
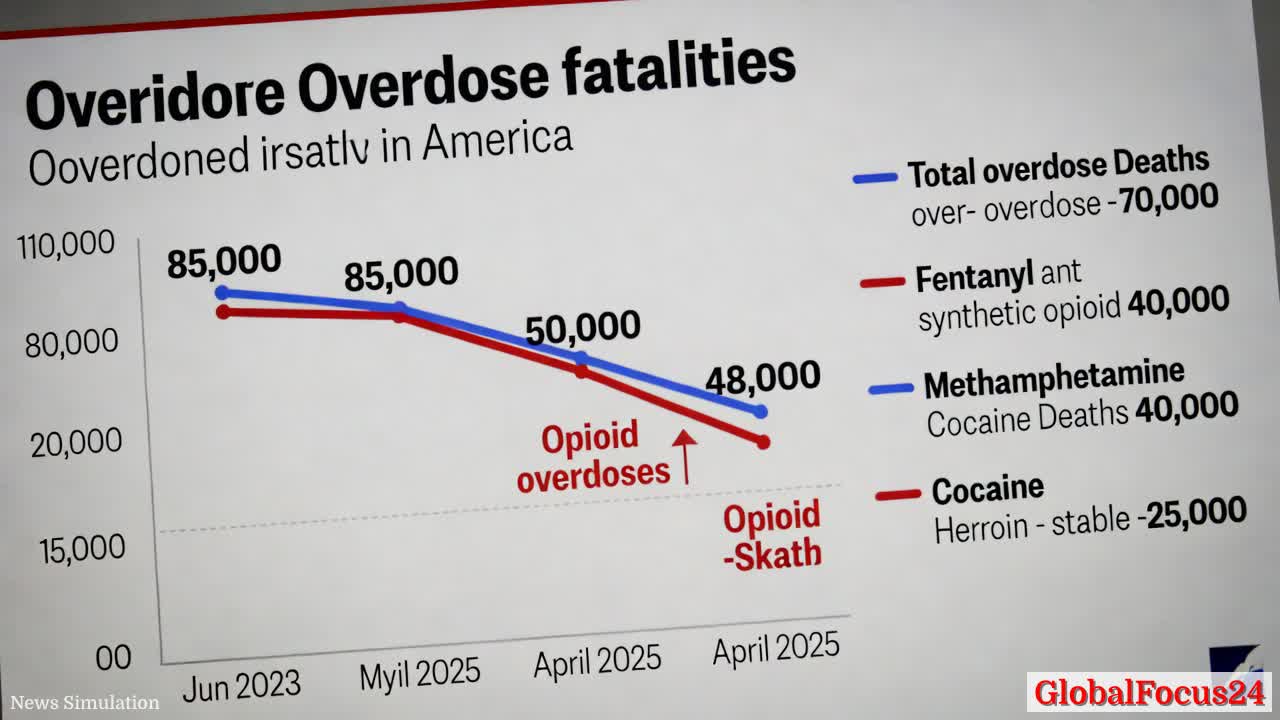
Since that 2023 peak, the trend has shifted dramatically. Preliminary figures for 2025 show that total overdose deaths have fallen to approximately 70,000. The change is most evident in fatalities linked to opioids, which plummeted from nearly 85,000 in mid-2023 to around 48,000 in the 12 months ending April 2025. This represents the fastest drop in overdose mortality rates since national records began tracking synthetic opioid deaths at scale.
While psychostimulant-related deaths—primarily those tied to methamphetamine—continue to rise modestly, reaching about 40,000 in 2025, and cocaine-linked deaths remain steady near 25,000, the overall decline is powered by one development: a sharp contraction in deaths involving fentanyl and other synthetic opioids.
The Fentanyl Saturation Effect
One leading explanation for the decline lies in what researchers describe as a “supply saturation” in the fentanyl market. After years of rapid growth, the market for illicit fentanyl may have reached peak penetration by 2023. As supplies became ubiquitous and doses ever more potent, the population of users at highest risk began to shrink—due to both mortality and shifts in consumption behavior. In practical terms, the tragic loss of some of the most vulnerable users, combined with growing fear of fentanyl’s unpredictability, reduced overall exposure.
Additionally, law enforcement disruptions of fentanyl trafficking networks—from cross-border operations to domestic pill press seizures—have limited distribution channels. Data from the U.S. Drug Enforcement Administration indicate that fentanyl seizures reached record highs in 2023 and early 2024, suggesting that much of the illegally manufactured supply never reached retail markets.
The Role of Harm Reduction and Public Health
Parallel to these changes in supply have been systematic expansions in harm-reduction strategies and addiction treatment access. Widespread distribution of naloxone, the overdose-reversal medication, has saved countless lives. In many states, community organizations hand out naloxone free of charge and train laypeople to use it effectively. Public awareness campaigns have increased recognition of fentanyl’s dangers and the importance of testing drugs before use.
Pharmacies across much of the country now sell rapid fentanyl test strips, while supervised consumption centers—where individuals can use substances in controlled environments—have launched pilot programs in major cities like New York and Philadelphia. At the clinical level, access to medication-assisted treatment (MAT) for opioid-use disorder, including buprenorphine and methadone, has expanded significantly following pandemic-era policy changes that allowed telehealth prescribing.
These public health measures, experts suggest, have produced measurable improvements in survival rates even when overdoses occur. The growing integration of addiction care into general healthcare systems, rather than siloed specialty clinics, is also helping normalize treatment and reduce stigma.
Regional Variations in Recovery
Although the national numbers tell a hopeful story, the decline is unevenly distributed across the country. States in the Northeast and Pacific Northwest, which faced fentanyl crises earlier and more intensely, are now seeing some of the steepest declines. For example, preliminary state-level analyses indicate that overdose deaths in Massachusetts, Rhode Island, and Washington fell by more than 30 percent between 2023 and 2025.
In contrast, parts of the South and Midwest—particularly states like Tennessee, Indiana, and Missouri—are experiencing smaller improvements or even slight increases in stimulant-related deaths. In these regions, methamphetamine and counterfeit pill distribution remain pervasive, underscoring how America’s drug crisis has splintered into multiple, co-existing epidemics.
Border states have seen unique dynamics as well. Enhanced collaborations between U.S. law enforcement and Mexican authorities have intercepted larger quantities of precursor chemicals used to synthesize fentanyl, particularly in border-crossing corridors such as Laredo, San Diego, and Nogales. Yet these enforcement gains are balanced against concerns about market substitutions, as producers pivot toward other synthetic drugs, including emerging analogs not yet explicitly scheduled under U.S. law.
Economic Impact of a Declining Crisis
The economic toll of the opioid epidemic has been staggering—by some estimates surpassing $1 trillion annually in lost productivity, healthcare costs, and criminal justice expenditures at its height. A sustained fall in overdose deaths not only signals improved public health but may also bring significant economic relief to families, healthcare systems, and local governments.
Fewer emergency interventions and hospitalizations translate into reduced strain on healthcare infrastructure. Employers report fewer workforce disruptions due to substance-use-related absenteeism. Communities that once bore the full weight of the crisis, including those in Appalachia and the Rust Belt, are beginning to reallocate resources toward long-term recovery projects and mental health services rather than solely emergency response.
Moreover, the conclusion of several high-profile opioid litigation cases, resulting in multi-billion-dollar settlements from pharmaceutical companies and distributors, has infused funding into treatment, prevention, and recovery initiatives. These investments are beginning to yield visible outcomes at the neighborhood level—rehabilitation facilities expanding capacity, community centers offering addiction counseling, and local governments rebuilding support systems torn apart by years of tragedy.
Lessons from History and Abroad
To fully understand the turnaround, it helps to view it in the broader context of drug-epidemic histories. The U.S. experienced similar waves in earlier decades—the heroin crisis of the 1970s, the crack epidemic of the 1980s, and the prescription opioid surge of the 2000s. Each episode followed a pattern: an explosive rise in availability and addiction, followed eventually by stabilization through market saturation, shifts in consumer behavior, and public health interventions.
Internationally, similar patterns have emerged. In Portugal, for instance, a radical decriminalization and treatment-centered model introduced in 2001 led to significant declines in overdose deaths within a decade. Canada’s western provinces, which faced their own fentanyl outbreak earlier than the U.S., have recently reported modest declines as well, aided by expanded harm-reduction policies and safe supply programs. These comparisons highlight how policy flexibility and sustained investment can meaningfully reshape outcomes over time.
Challenges Ahead
Despite the promising data, experts caution that the battle is far from over. The persistence of psychostimulant-related deaths, along with the emergence of new synthetic compounds such as nitazenes, underscores the unpredictable nature of the illicit drug supply. Some regions are now reporting increasing use of xylazine, an animal tranquilizer often mixed with fentanyl, which complicates overdose treatment.
Additionally, while overdose deaths have declined, addiction remains widespread. Millions of Americans continue to struggle with substance-use disorders, and relapse rates remain high. Sustaining the current gains will require keeping treatment accessible, strengthening community-based prevention programs, and continuing to monitor new threats from emerging synthetic drugs.
A Turning Point with Cautious Optimism
The decline in overdose deaths is one of the clearest indicators that long-term public health strategies, combined with shifts in the drug market, are working. After years of devastation, America appears to be approaching a new chapter in the fight against overdose fatalities. The numbers suggest a nation beginning to stabilize after an unprecedented wave of loss—but experts emphasize that progress can slip if vigilance wanes.
The challenge now is to build on momentum—not to declare victory, but to ensure that shrinking mortality rates translate into resilient recovery for individuals, families, and communities alike. In the long arc of America’s struggle with addiction, 2025 may be remembered as the year the tide finally began to turn.